Shoulder Surgery
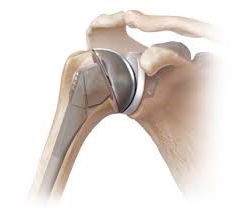
Total Shoulder Replacement
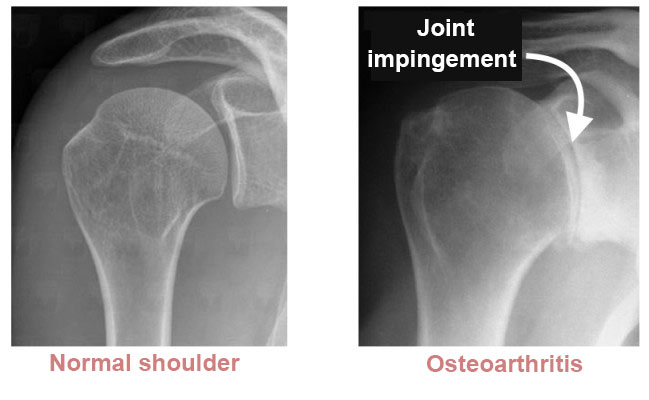
Osteoarthritis of the shoulder is a degenerative condition that affects the shoulder joint. It causes pain and stiffness that get worse over time. A shoulder replacement can treat the pain and restore normal movement. There are different procedures (anatomic or reverse total arthroplasty) depending on the type of osteoarthritis. A joint replacement may also be needed for necrosis or a fractured shoulder. Necrosis of the humerus is also an indication for shoulder replacement surgery.
Contents
- Video presentation
- Description & progression
- Diagnosis & Surgical indication
- Preparing for surgery
- Hospital stay & procedure
- After the surgery & results
- Potential complications
Osteoarthritis of the shoulder happens when the surfaces inside the shoulder joint become worn and the cartilage gradually disappears. This wearing away gets worse over time, causing abnormal friction, pain, swelling (fluid accumulation and bursitis) and stiffness (limited movement in the shoulder). The pain happens not only when you move the shoulder, but also and often more disturbingly, at night. The wearing away of the cartilage is irreversible, and there is no cure for osteoarthritis. The only thing you can do is slow it down.
Osteoarthritis is a degenerative condition, which means it is linked to wear and tear, but there are also extrinsic factors that can accelerate the progression of the disease. The main causes are:
- A history of recurrent shoulder dislocation
- A rotator cuff tear
- Surgery on the shoulder joint
- Fracture (of the humerus or glenoid rim (shoulder blade))
- A rheumatic disorder (e.g. chondrocalcinosis, rheumatoid arthritis)
The first step in treating osteoarthritis is to give medical treatment i.e. pain relief. This is often combined with hygiene and dietary measure to alleviate the pain. Injections of hyaluronic acid are also required to lubricate the joint and protect the damaged cartilage. This is sometimes combined with physical therapy.
There are two types of shoulder osteoarthritis :
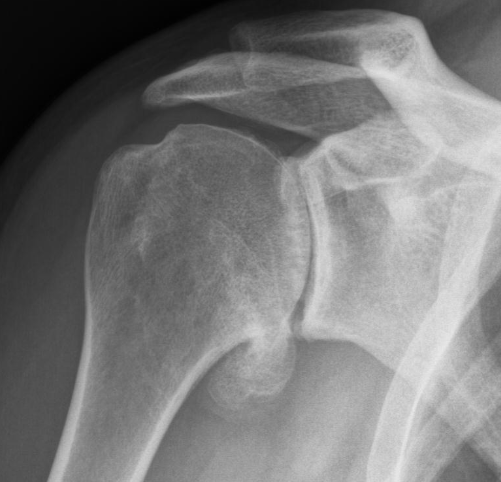
Concentric (primary) :
This is the standard form of osteoarthritis where the cartilage has worn away from the head of the humerus and glenoid rim. The rotator cuff tendons are intact and still working. It usually affects patients in their sixties. X-rays reveal a humeral head nicely centred within the joint, and an MRI confirms no damage to the rotator cuff tendons.
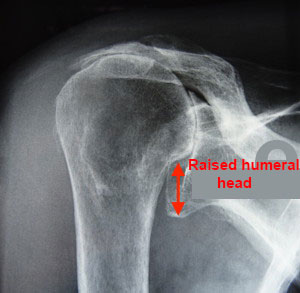
Eccentric (secondary) :
This is a particular form of osteoarthritis where the rotator cuff tendons have been torn. The humeral head is no longer held in place by the tendons and moves off-centre. X-rays show the humeral head raised above the glenoid rim of the shoulder plate. An MRI confirms a rotator cuff tear.
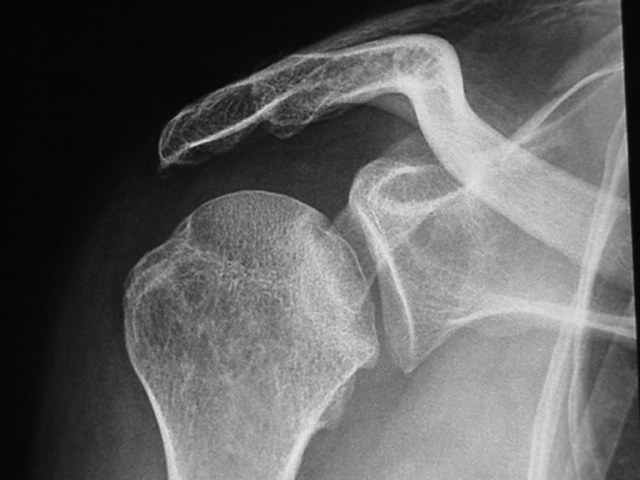
Osteonecrosis of the humeral head :
Osteonecrosis of the humeral head is a complication of a bone infarction, which can have wide-ranging causes (steroid therapy, haemoglobin disorders, Lupus or other auto-immune diseases) or even no known cause. It causes pain and stiffness. The condition can be diagnosed with standard x-rays for advanced cases, or with an MRI for early cases.
Treatment is always surgery.
Surgery is indicated when medical treatment no longer has any effect.
It involves a total shoulder replacement.
The diagnosis is based on the clinical history, with patients often clearly describing pain for many years and a gradual loss of range of motion in the joint. The night pain becomes more and more disabling. There is often an identifiable cause (e.g. dislocation, shoulder surgery, rotator cuff tear).
An x-ray is essential for confirming the diagnosis. The images are taken from the front with the joint in three rotations (lateral, medial and neutral) and from the side. They reveal joint impingement i.e. a narrowing of the distance between the joint surfaces indicating loss of the cartilage.
Multi-slice imaging (MRI or joint scan) will also be used to determine the extent of damage to the rotator cuff and plan any surgery.
These results will be used to classify the osteoarthritis as concentric or eccentric.
A Total Shoulder Replacement is indicated when medical treatment no longer has any effect. The procedure offers functional treatment with the sole aim of improving the patient’s quality of life. It is therefore ultimately up to the patient to decide whether to go ahead with the operation. Dr Lévy will try to explain what will happen in either scenario, with and without the surgery. Surgery should be recommended for patients whose daily lives are disabled by the shoulder pain, especially if the night pain is preventing the patient from sleeping. This disability should be significant, and not just occasional. There is no hard and fast rule, because every patient is different. There is no age limit for a total shoulder replacement, but it should be avoided in young patients because the only limitation of the procedure is the life span of the implants which will eventually have to be replaced if the patient is too young; although sometimes, there is obviously no other option. Fortunately, there have been great improvements in implant quality and they now have a much longer life span.
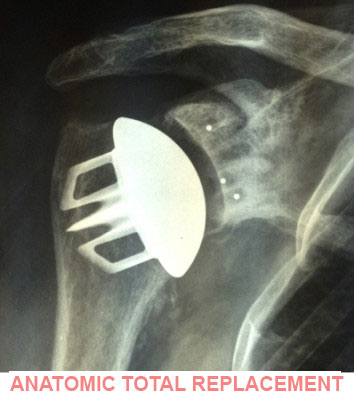
For concentric osteoarthritis, Dr Lévy will use a technique known as an anatomic total shoulder replacement. The implant works the same as a normal shoulder but needs the rotator cuff tendons to be intact. The tendons are what will allow the shoulder to move after the surgery. If the rotator cuff tendons are torn, the implant will not work.
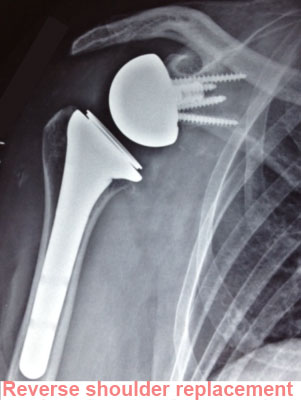
For eccentric osteoarthritis, he will use a reverse total shoulder replacement. This is a special type of implant that changes the centre of rotation of the joint, allowing the shoulder to work without the need for the rotator cuff tendons. The deltoid muscle does all the work, allowing the shoulder to still move. Unfortunately, this type of implant has a shorter life span than anatomic implants.
Ultimately, the need for surgery will be decided after a long discussion between the patient and surgeon.
SURGICAL CONSULTATION:
The aim of the preoperative consultation with the surgeon is to establish a diagnosis. Dr Lévy will examine the shoulder to determine how much the joint is damaged. A clicking sound when moving the shoulder could be a sign that the cartilage has worn away and the end of the humerus bone is rubbing against the glenoid rim. The shoulder will have very limited movement and be very painful.
The surgeon will use X-rays and other tests to confirm the diagnosis and plan the surgery. Depending on the damage and its cause, Dr Lévy will decide what is required. He will explain what will happen during and after the surgery, as well as any potential complications. This will include a discussion of the recovery time and any rehabilitation required after the operation.
You will be given time to discuss your options, and you will receive advice on the pros and cons of the surgery.
Once a decision has been made, Dr Lévy will take some blood and urine samples in order to make sure you have no infection. He will ask for a dental panoramic x-ray to rule out a dental infection. He will also need an echo Doppler scan of the neck to check for any damage to the carotid arteries. You will have to see a cardiologist and get their go-ahead for the surgery. Finally, you will have an appointment with the anaesthetist.
ANAESTHETIC CONSULTATION:
Once the indications have been confirmed, one of Dr Lévy’s assistants will give you an appointment with the anaesthetist who will look after you during the operation. The anaesthetist will examine you and prescribe any additional tests that may be needed before the surgery. He or she will also explain how the anaesthesia works and the best method for you. The operation is usually carried out under general anaesthesia, together with a regional catheter for managing the pain immediately after the procedure.
SMOKING :
It is essential to stop smoking one month before and after the surgery. This is because a mass influx of nicotine reduces blood flow and slows down the healing process. You may use extended-release nicotine patches to help with the withdrawal symptoms.
You will stay in hospital for about five days. This time is needed to treat the initial pain, monitor the wound and start your rehabilitation.
The procedure is usually performed under general anaesthesia. It takes between 60 and 90 minutes. The surgeon will make an incision into the shoulder using the deltopectoral approach. Next, he cuts the pectoralis major muscle in order to access the shoulder (subscapular). The surgeon will then make a cut in the head of the humerus to get to the shoulder blade. Any remaining cartilage is removed from the shoulder blade, then the glenoid implant is put in place. This is a precision operation, and perfect implant size is chosen for each individual patient. Dr Lévy uses cutting guides and ultra-precision instruments to place the implant in exactly the right position, based on the plans made in advance.
There are two or three parts to the implant:
- One humeral component made of chrome/cobalt
- One glenoid component made of polyethylene for an anatomic procedure, or two metal components for a reverse procedure
The surgeon will carefully secure haemostasis (cauterise the blood vessels) to keep the blood loss to a minimum. He will take care to suture the subscapularis muscle before closing the skin. A process called autologous blood transfusion is often used – the blood shed during the surgery is centrifuged, concentrated, then reinfused back into the patient to avoid the need for a subsequent blood transfusion. Autologous transfusions are safe because they use the patient’s own blood. There is therefore no risk of contamination or rejection.
ANATOMIC TOTAL REPLACEMENT :
REVERSE TOTAL REPLACEMENT :
Video coming soon…
Once the operation is finished, you will be transferred to the recovery room where your vital signs and pain levels will be monitored. Any autologous transfusion will take place in the recovery room. You will spend about two hours there.
Then you will return to your room to rest. The next day, the nurses will administer any painkillers prescribed by the anaesthetist, and you will receive a visit from the physiotherapist to start your rehabilitation. Th exercises will focus on gently mobilising the shoulder (pendulum movements and anterior elevation but without any lateral rotation (for one month) to avoid reopening the subscapularis muscle. You will receive a private physiotherapy session every day. For some of the first day, you will be allowed to sit up in a chair.
You will usually be discharged to a rehabilitation centre for several weeks, but you may also be allowed to return home and receive daily visits by nurses, support workers and physiotherapists under the PRADO protocol, a scheme introduced by the Department of Social Security to help patients return home after an operation.
You should keep your arm in a sling night and day for 4 weeks after the surgery. If you are very careful or when taking a shower, you can remove your arm from the sling and hold it against your body. Rehabilitation will start as soon as possible, with the aim of keeping the joint mobile. It will start with pendulum exercises several times each day. The only movement you are not allowed to do during the first month is lateral rotation (turning the arm outwards). Nurses will come to change your dressing for 2–3 weeks. You should do your exercises every day to help your shoulder recover as much mobility as possible. The skin staples will be removed between day 1 and 21.
POSTOPERATIVE CHECK-UPS :
30-DAY CHECK-UP :
By now you will have started physiotherapy to help restore the range of motion in the joint. The swelling should have begun to go down a little bit, and it will be less painful. The night pain should in principle have disappeared. Dr Lévy will examine the scar, your mobility, and determine whether there is any residual pain. He will look at your new x-rays, and make any necessary adjustments to your recovery plan for the next few months. You should be able to start driving again after 45 days.
4-MONTH CHECK-UP :
Your rehabilitation should now be aimed at restoring full range of motion, including rotation, and supporting the muscles. You should be getting used to your implant, but will still be aware it is there. Your muscles will not quite have regained full strength, and you can improve it with either exercises at home or physiotherapy. Dr Lévy will give you advice on how to avoid damaging the shoulder.
Depending on your recovery, he may allow you to resume running, cycling and swimming.
12-MONTH CHECK-UP :
In principle, by now you should no longer have any pain and be able to move your shoulder however you want, without thinking about it. However, each shoulder is different and Dr Lévy will give you specific advice on whether you can resume sports. It is possible to play many sports after a total shoulder replacement (e.g. tennis, golf, skiing, running). Your surgeon will give you a schedule for gradually resuming these activities. Contact sports (e.g. football, rugby, judo) should be avoided.
RESULTS :
Shoulder replacement surgery gives an excellent result in over 90% of cases, with patients experiencing no or very mild pain. Patients will often forget about their total shoulder replacement within 6–12 months.
The average life span for a total shoulder replacement is 15–20 years for anatomic implants, and 10 years for reverse implants. After this time it will need to be replaced. The second operation is often more complicated than the first time, and the results not quite as good.
You should see your surgeon for a check-up every year, with x-rays to check for any complications. This will just be a short appointment so he can check the scar, your movement, any pain and take some x-rays.
You must take every precaution against infections, and treat any infection as quickly as possible (dental, sinus, urinary infections etc.). This is because the bacteria could migrate to the shoulder at any time and infect the implant, in which case the only option will be to have it replaced.
A wide range of complications can occur with surgery. Fortunately, they are very rare and the various appointments before and after the surgery are designed to avoid them, or detect them early if they do appear.
As well as the risks common to all types of surgery and the risks of the anaesthesia, there are some specific risks associated with this procedure.
The following complications may occur with shoulder replacement surgery:
SURGICAL SITE HAEMATOMA :
A haematoma is a rare but serious complication. Haematoma happens when there is bleeding from a small vessel in the shoulder, filling the space with blood. The shoulder swells and becomes painful and taut. If the cavity gets too swollen, the surgeon may have to perform a joint aspiration. If it happens again, it may require further surgery to locate the leaking blood vessel and cauterise it.
SURGICAL WOUND INFECTION :
Despite all the precautions taken by the operating team, bacteria may still enter the wound either during the surgery or afterwards, before it is fully healed. This compromises the healing (more redness around the wound than normal), causing severe pain, a purulent discharge and a persistent fever.
You must tell the surgeon if you see any of these signs and seek EMERGENCY treatment.
DO NOT TAKE ANY ANTIBIOTICS BEFORE SEEING THE SURGEON
Dr Lévy will decide whether to wash out the shoulder and send any samples for testing so he can prescribe the correct antibiotic for any infection, assuming it has been caught in time. Otherwise, the implant will have to be replaced. This is a major operation to treat the infection and can mean the functional results are not as good as was originally expected. You will also have to take antibiotics for at least 45 days and have regular check-ups with the surgeon. It is a serious complication.
PHLEBITIS/PULMONARY EMBOLISM :
This is a rare complication for upper limb surgery, when a blood clot forms in a vein (phlebitis) and requires long-term curative anticoagulant therapy.
JOINT STIFFNESS :
This can be a knock-on effect of inflammation (algodystrophy) and requires targeted physiotherapy. If you have not regained your full range of motion after three months, it could be caused by fibrosis which requires surgery.
COMPLEX REGIONAL PAIN SYNDROME :
Complex Regional Pain Syndrome, also called algoneurodystrophy, is a condition involving pain and other unpleasant symptoms in a joint after surgery or a fracture. The syndrome may have a neurological cause such as damage to the peripheral nervous system, affecting either the small fibres which protect from pain or heat stimuli, and/or the large fibres which detect tactile stimuli. It causes pain and severe stiffness that can last for up to 18 months. Patients always recover fully. Dr Lévy will diagnose the condition using scintigraphy (a scan) and will support you throughout, in order to treat the painful and unpleasant symptoms.
IMPLANT LOOSENING :
This is not a complication but a natural problem as the implant gets older. After several years, the implant can become loose and cause pain. It will need to be replaced. An undetected infection could cause an implant to loosen sooner than expected. This is known as septic loosening. The surgeon will always check for an infection in case of early loosening.
ROTATOR CUFF TEAR :
After an anatomic replacement, the risk of a rotator cuff tear is the same as for a native shoulder. If this happens, the implant will need to be removed and replaced with a reverse design.
IMPLANT DISLOCATION :
Although rare, the implant may dislocate and the joint come out of its socket. It is important to investigate the cause (e.g. trauma, rotator cuff tear, loosening).
This list does not cover all the possible risks.
Ask Dr Lévy if you want more information, especially if you have any questions about your particular situation and the advantages, disadvantages and risk/benefit ratio of each procedure.