Forefoot surgery
Morton’s Neuroma
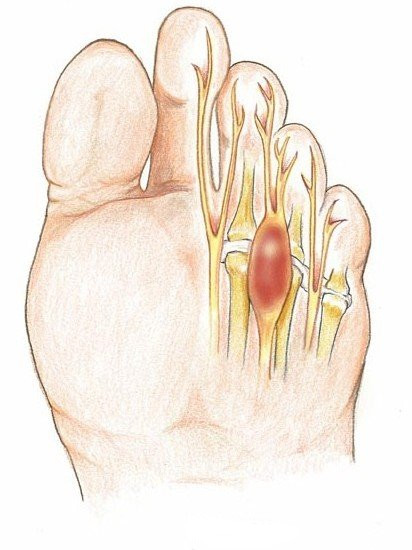
Morton’s Neuroma is a painful foot condition caused by compression of a nerve between two metatarsal bones. This compression causes inflammation of the common digital plantar nerve, a condition known as Morton’s Neuroma. Sufferers experience searing pain that feels like an electric shock radiating into the toes. Surgery can treat the condition but is a last resort after other non-surgical treatments.
Dr Lévy treats Morton’s Neuroma using a percutaneous minimally-invasive technique.
Contents
- Description & progression
- Treatment
- Preparing for surgery
- Hospital stay & procedure
- After the surgery
- Recovery period & Return to work
- Potential complications
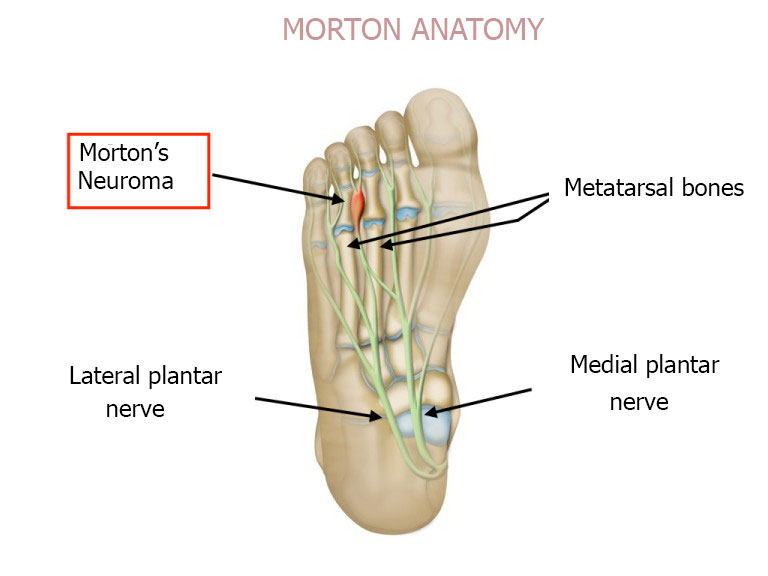
Morton’s Neuroma (also known as Morton’s metatarsalgia or interdigital neuroma) is a pseudo-tumour that grows along a nerve on the sole of the foot. The neuroma occurs at the anastomosis (a point where two nerves merge to form a larger nerve) between the two nerves responsible for feeling in the sole of the foot: the medial plantar nerve and the lateral plantar nerve.
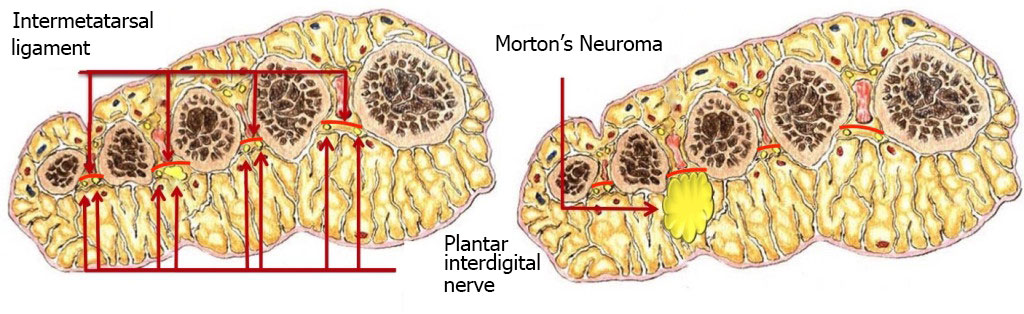
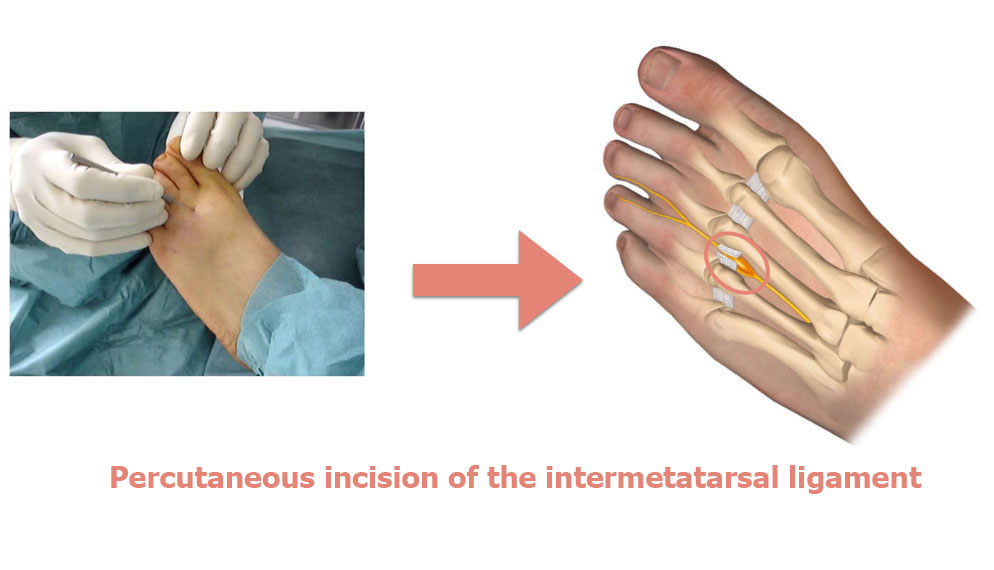
It compresses the nerve between the third and fourth metatarsal, causing it to become inflamed. This inflammation leads to a neuroma, which itself get squeezed between the two bones, making the inflammation even worse. The result is a vicious circle. In fact, the space between the two bones cannot get any wider because the intermetatarsal ligament is not stretchy. Therefore the main aim of surgery is to cut the intermetatarsal ligament in the space affected by the neuroma.
PATHOPHYSIOLOGY OF MORTON’S NEUROMA
SYMPTOMS OF MORTON’S NEUROMA
The main symptom is searing pain similar to burning, usually originating in the third metatarsal space (between the base of the third and fourth toes). A Morton’s Neuroma can also grow in the second metatarsal space. The pain, which radiates out to the side of the toes, is felt when standing or walking. Sufferers are often forced to take their shoes off to relieve the pain and are no longer able to wear narrow footwear.
MORTON’S NEUROMA NEVER CAUSES PAIN WHEN BAREFOOT.
The burning pain is often accompanied by pain on the sole of the foot, feeling like you’re walking on pebbles. This is caused by the metatarsal heads pressing against the ground due to loss of the soft protective pad between the skin and bone. Eventually, the compression from the neuroma can lead to partial or even complete loss of feeling in the toes affected.
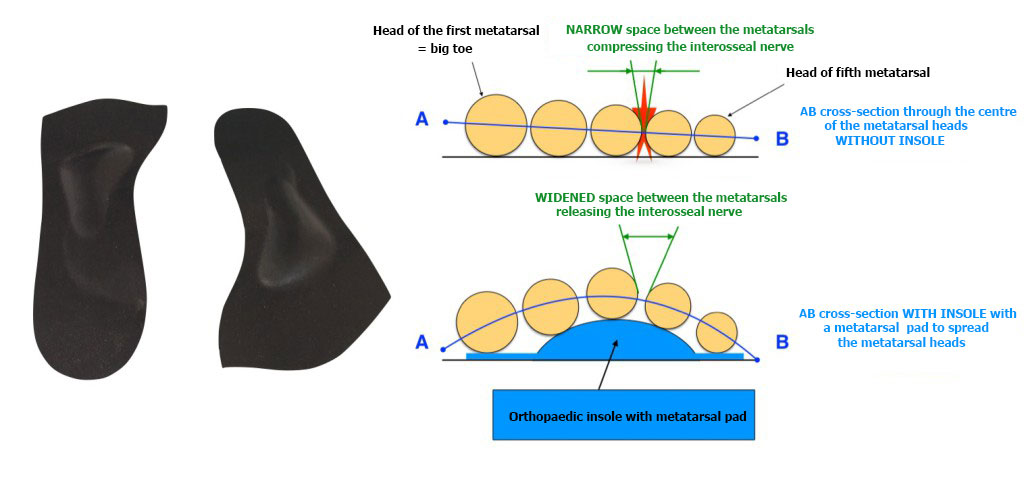
Morton’s Neuroma should always first be given medical treatment. The pain can usually be effectively relieved by wearing orthopaedic insoles SPECIALLY DESIGNED for metatarsal conditions.
Patients often wear the wrong sort of insoles. These do not work. The aim of the insoles is to relieve the pressure on the nerve by spreading the metatarsal bones.
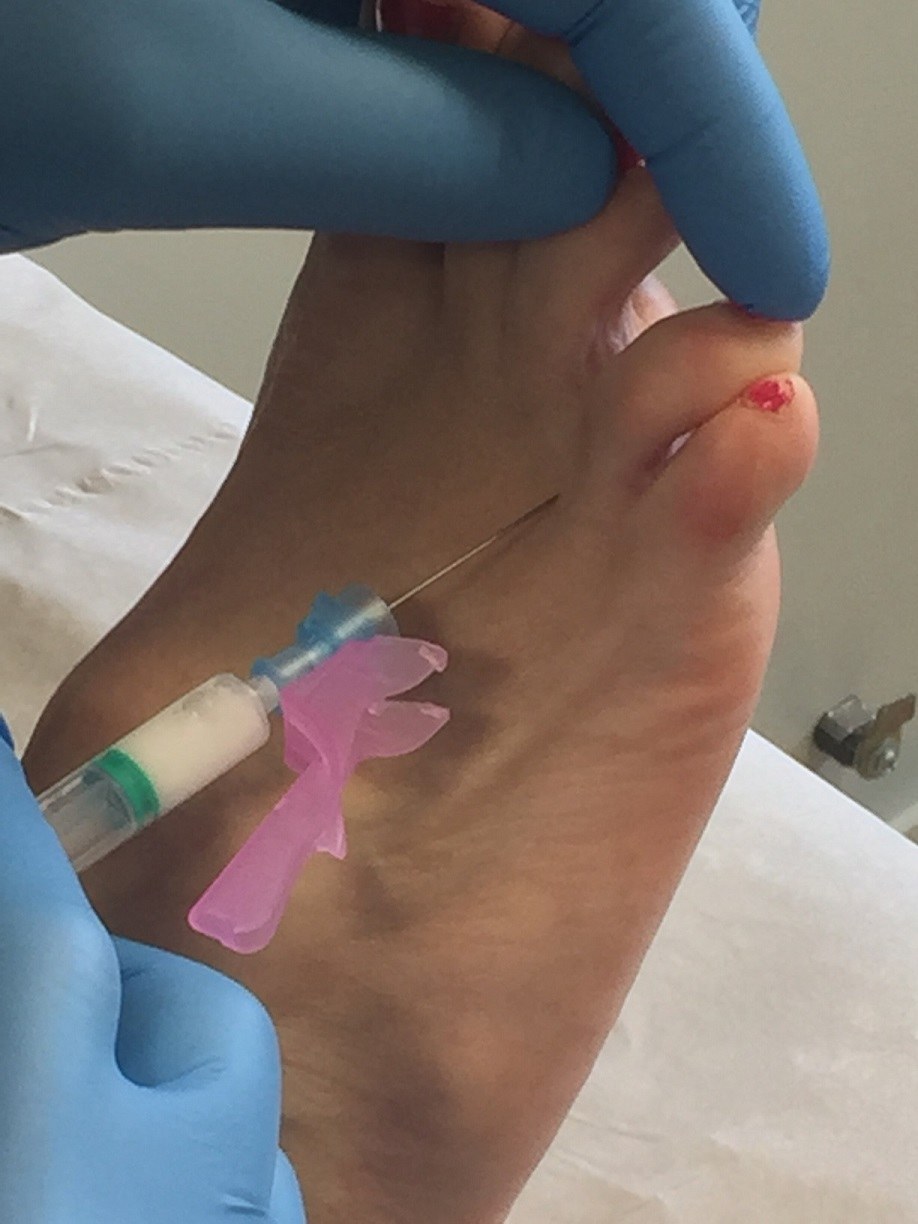
If the correct insoles are being worn properly but the pain persists, an injection can be given into the area of the neuroma. This steroid injection can be performed by the surgeon during an appointment at the clinic. The aim is to break the vicious circle of inflammation and compression. Reducing the inflammation around the neuroma makes it shrink and, using insoles to spread the metatarsal bones, the neuroma then heals, and the pain disappears.
In rare cases, medical treatment does not work. Surgery is then required. Most surgeons decide to remove the neuroma and the related nerve. The aim is to alleviate the searing pain, but it does mean the patient will lose all feeling in the end of the third and fourth toes. In addition, this method does not treat any associated pain caused by the metatarsal heads pressing on the ground. This means the plantar pain will not go away.
Dr Lévy treats neuromas by targeting the compression on the bones without touching the nerve. He uses percutaneous surgery to make more space for the nerve. The benefit of this technique is that it does not leave scars, and it not only treats the Morton’s Neuroma but also the pressure pain. Furthermore, by leaving the nerve intact, the patient does not lose feeling in the toes. The disadvantage is the amount of time needed off work, and the longer postoperative swelling.
SURGICAL CONSULTATION:
During the presurgical consultation, Dr Lévy will establish a diagnosis and make sure that the medical treatment has in fact failed despite being correctly followed. He will examine the structure of your foot to see whether it is flat or hollow. Any deformity will have to be addressed after the surgery using orthopaedic insoles. The foot will also be checked for hammer toe or mallet toe, which can be treated at the same time.
X-rays will be used to help plan the surgery. The surgeon will decide what is required based on the deformity and the x-rays. He will explain what will happen during and after the surgery, as well as any potential complications.
ANAESTHETIC CONSULTATION:
Once the indications have been confirmed, one of Dr Lévy’s assistants will give you an appointment with the anaesthetist who will look after you during the surgery. The anaesthetist will examine you and prescribe any additional tests that may be needed before the surgery. He or she will also explain how the anaesthesia works and the best method for you.
SMOKING :
It is essential to stop smoking one month before and after the surgery. This is because a mass influx of nicotine reduces blood flow to the foot and makes it harder for the bone to heal, causing prolonged pain. You may use extended-release nicotine patches to help with the withdrawal symptoms.
The surgery is usually carried out as an outpatient procedure (day hospital).
ANAESTHESIA :
The procedure will be performed under local anaesthesia. The anaesthetist will first give you a local anaesthetic into the ankle and top of the foot so you won’t feel any pain or discomfort during the surgery. Further anaesthesia will be given directly into the toes being operated. This top-up is used to prolong the effects of the anaesthesia for 10–12 hours. You will therefore not be in any pain when you return home. When you are discharged from the clinic, you will be given a prescription for pain relief.
PERCUTANEOUS SURGERY :
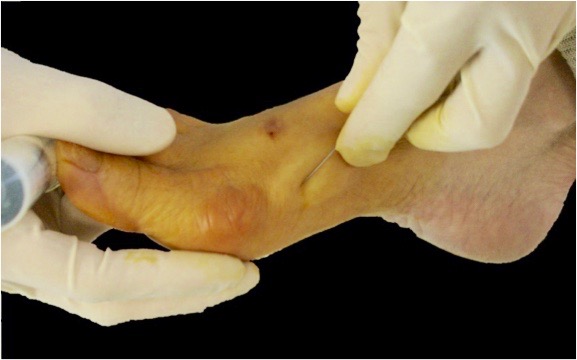
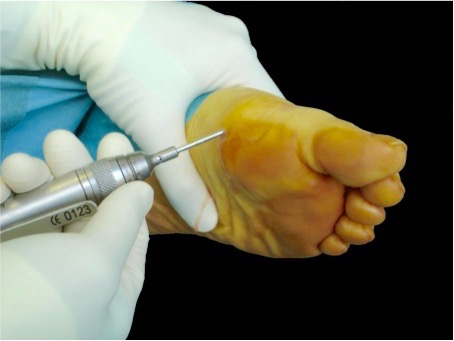
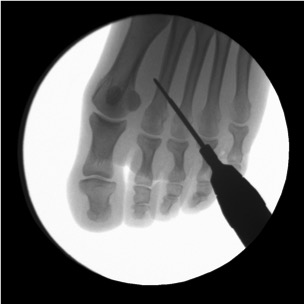
The surgeon will perform the metatarsal osteotomy by making micro-incisions for inserting instruments just 2mm in diameter. This means the scars will be barely visible to the naked eye. Dr Lévy will cut the intermetatarsal ligament joining the two metatarsal bones and causing the compression.
Next he performs an osteotomy (removing part of the bone) for the second, third and fourth metatarsal, using oblique cuts to spread and raise the metatarsal heads. This decompresses the nerve and reduces the pressure of the bones on the floor. No stitches are required. No fixation material is used (e.g. screws, staples).
Throughout the operation, the surgeon will take x-rays to check what is happening and make sure the osteotomy is as accurate as possible.
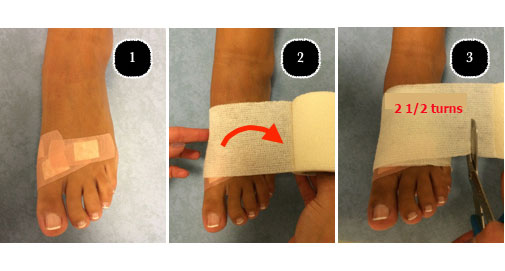
Once finished, he will apply a compression dressing that will act as a splint for 8–10 days, during which you should not remove or loosen the bandage or get it wet.
You will then spend a few minutes in the recovery room so your vital signs can be monitored, before returning to your room and waiting to be discharged.
Dr Lévy will prescribe any medication needed to alleviate any pain after the surgery. When you are discharged, you will be given a copy of your medical file explaining that you must bring back the dressings to your next check-up, along with any other instructions and the date and time of your next appointment when you will have another x-ray.
After being discharged, you will be able to walk with orthopaedic shoes that Dr Lévy will have prescribed for you during the preoperative consultation.
The surgeon will give you an appointment for a check-up in 8–10 days’ time. During this time, you must wear the orthopaedic shoes which are designed to relieve pressure on the forefoot.
POSTOPERATIVE CHECK-UPS :
8–10 DAY CHECK-UP :
Dr Lévy will remove the dressing, check the realignment, examine your x-rays and make sure the wound is healing. He will give you a splint to keep the bones in place and make sure the deformity does not return. This splint will make sure the bones heal in the correct position. You must wear it for 3 weeks. The dressings will be changed every three days until your next appointment. You must wear orthopaedic shoes for one month.
1-MONTH CHECK-UP :
The dressing and splint will be removed. You will return the orthopaedic shoes and can start wearing loose–fitting footwear (e.g. trainers, plimsolls). The swelling usually takes about 3 months to go down. Dr Lévy will give you compression bands which you must wear every day for three months after the operation. You will also be given some exercises to do at home to help recover the full range of motion in your toes.
3-MONTH CHECK-UP :
This is a simple check-up to see how you are doing. However, each case is different and you may be given advice on how to improve your condition and speed up your recovery.
You may also be given further appointments, if the surgeon thinks it is necessary.
REHABILITATION :
The benefit of percutaneous surgery is less stiffness after the procedure. In most cases there is no need for physiotherapy. At your first check-up appointment, Dr Lévy will give you some exercises to do at home. These exercises are designed to restore the range of motion in the joints, massage the scars to prevent any deep-seated adhesions, and get you walking again normally.
In some cases, he may want to prescribe you some sessions with a physiotherapist.
The length of time you need to take off work will depend on your job and how you travel to get there. After an osteotomy, the swelling lasts for an average of three months.
You should not drive for six weeks (unless you have an automatic car and operate the pedals using the other foot). Likewise, you should not expect to be able to walk for long distances for at least six weeks.
For example, if you work in an office located 5 minutes from your house, you can expect to return to work within a month, or possibly even one week after the surgery. On the other hand, if you have a physically active job with a 2-hour daily commute, you may need to take up to three months off. These are just two examples, and your situation may lie anywhere in between.
A wide range of complications can occur with surgery. Fortunately, they are very rare and the various appointments before and after the surgery are designed to avoid them or detect them early if they do appear.
As well as the risks common to all types of surgery and the risks of the anaesthesia, there are some specific risks associated with this procedure.
The following complications may occur with percutaneous surgery of the foot :
SURGICAL WOUND INFECTION :
Despite all the precautions taken by the operating team, bacteria may still enter the wound either during the surgery or afterwards, before it is fully healed. Signs and symptoms of an infection are compromised healing with severe pain, more redness around the wound than normal, a purulent discharge and a persistent fever.
You must tell the surgeon if you see any of these signs and seek emergency treatment.
DELAYED HEALING :
Sometimes, the bones take longer than three months to heal. This is often the case with smokers who were unable to quit before, during and/or after the surgery due to the decreased blood flow to the toes. In these cases, Dr Lévy will give you advice on how to reduce pressure on the bones and help them heal faster.
COMPLEX REGIONAL PAIN SYNDROM :
Complex Regional Pain Syndrome, also known as algodystrophy, is a condition involving pain and other symptoms usually in a limb following trauma or surgery, even if only minor. The syndrome may have a neurological cause such as damage to the peripheral nervous system, affecting either the small fibres which protect from pain or heat stimuli, and/or the large fibres which detect tactile stimuli. It causes pain and severe stiffness that can last for up to 18 months. Patients always recover fully. Dr Lévy will diagnose the condition using scintigraphy (a scan) and will support you throughout, in order to treat the painful and unpleasant symptoms.
PHLEBITIS/PULMONARY EMBOLISM :
Despite walking again immediately after the operation, a clot may form in one of the veins of your leg (phlebitis) and require an effective dose of anticoagulant treatment for 3–6 months. This complication is rare with percutaneous surgery because the patient can walk again the same day.
FAILURE OR PERSISTENT METATARSAL PAIN :
In rare cases, an osteotomy does not successfully decompress the neuroma. If the pain persists, it is usually due to residual metatarsal pressure pain. In this case you will have to wear orthopaedic insoles. If the neuroma is still painful, you may have to consider a more conventional treatment i.e. surgical removal of the neuroma.
This list does not cover all the possible risks.
Ask Dr Lévy if you want more information, especially if you have any questions about your particular situation and the advantages, disadvantages and risk/benefit ratio of each procedure.