Home » Pathologies » Forefoot surgery » Hallux Rigidus
Hallux Rigidus
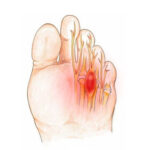
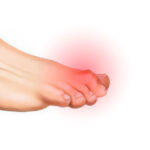
Hallux rigidus is the name given to primary osteoarthritis of the first metatarsophalangeal joint of the hallux (the joint at the base of the big toe). It’s a painful deformation caused by exostosis (bone growth) on the top of the foot, visible as a bump under the skin that rubs against shoes. The other clinical sign is stiffness. If medical treatment (injections) is unsuccessful, it can be treated with surgery.
Dr Lévy treats Hallux Rigidus using a percutaneous minimally-invasive technique called Halluxoplastie® procedure.
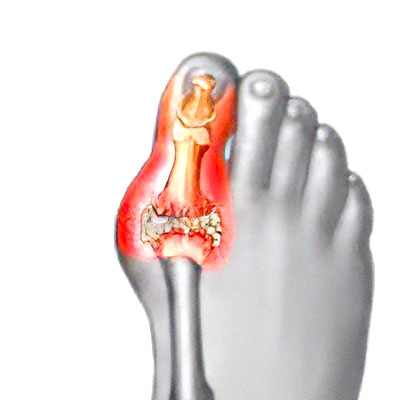
Description & progression
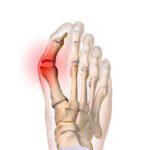
Hallux rigidus is the name given to primary osteoarthritis of the first metatarsophalangeal joint of the hallux (the joint at the base of the big toe). It is characterised by a bony growth (exostosis). This exostosis sits on top of the toe, protruding under the skin and rubbing against the shoe.
It causes pain when bending the metatarsophalangeal joint of the big toe. Patients experience stiffness i.e. they find it harder to move the joint. Walking is difficult and painful (even when barefoot) because the big toe cannot be straightened, obstructing our natural gait.
The three clinical signs are:
- STIFFNESS: loss of extension;
- PAIN: especially when pressing on the top of the joint;
- possible CORNS: due to rubbing against the shoe.
Hallux rigidus is often accompanied by another toe deformity known as Hallux Valgus. This combined condition is sometimes known as hallux rigido-valgus.
X-rays are used to confirm the diagnosis by revealing the usual signs of osteoarthritis: narrowing of the joint space, osteophytes, cysts and consolidation. Dr Lévy will also measure the angle of the metatarsal to determine the extent of any associated deformity (hallux rigido-valgus).
Treatment & Surgical indication
In the early stages of the condition, medical treatment may suffice, such as anti-inflammatories and painkillers.
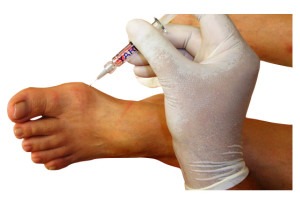
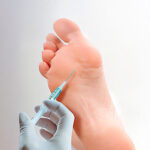
Steroid injections may be offered and can sometimes help. Injections of hyaluronic acid (viscosupplementation) may also be offered to lubricate the joint. Patients should try wearing different shoes to stop them rubbing against the skin.
If these treatments all fail, surgery may be required. There are various types of procedure depending on the type of problem. Dr Lévy treats hallux rigidus with percutaneous minimally-invasive surgery.
If the problems are caused by an exostosis i.e. the top of the bony bump rubbing against shoes, Dr Lévy will suggest a percutaneous technique to trim away the bump. This procedure is known as a cheilectomy.
If the problem is caused by pain when moving the first metatarsal against the first phalanx, permanent fusion will be needed to alleviate the pain. This procedure is known as arthrodesis. The surgeon will fuse the joint (which is already very stiff) between the metatarsal and first phalanx. This removes the pain but the patient can no longer bend the joint. This treatment should therefore only be considered if there is decompensation in the second phalanx i.e. it is much more flexible than normal. In fact, if there has been long-term stiffness in the first joint, the second phalanx will often take over and become much more mobile to prevent a limp. Fusing the first joint does not therefore cause a limp.
Dr Lévy performs these two operations using a percutaneous minimally-invasive technique.
Preparing for surgery
SURGICAL CONSULTATION:
The aim of the preoperative consultation with the surgeon is to establish a diagnosis and analyse the deformity, the loss of function and check for any other pain that the patient may not have mentioned (e.g. plantar pain beneath the second toe). Dr Lévy will examine the structure of your foot to see whether it is flat or hollow. Any deformity will have to be addressed after the surgery using orthopaedic insoles. The foot will also be checked for hammer toe or mallet toe, which can be treated at the same time.
X-rays will be used to help plan the surgery. The surgeon will decide what is required based on the deformity and the x-rays. He will explain what will happen during and after the surgery, as well as any potential complications.
ANAESTHETIC CONSULTATION:
Once the indications have been confirmed, one of Dr Lévy’s assistants will give you an appointment with the anaesthetist who will look after you during the surgery. The anaesthetist will examine you and prescribe any additional tests that may be needed before the surgery. He or she will also explain how the anaesthesia works and the best method for you.
SMOKING :
It is essential to stop smoking one month before and after the surgery. This is because a mass influx of nicotine reduces blood flow to the foot and makes it harder for the bone to heal, causing prolonged pain. You may use extended-release nicotine patches to help with the withdrawal symptoms.
Hospital stay & procedure
The halluxoplastie® procedure is usually carried out as an outpatient procedure (day hospital).
ANAESTHESIA :
The procedure will be performed under local anaesthesia. The anaesthetist will first give you a local anaesthetic into the ankle and top of the foot so you won’t feel any pain or discomfort during the surgery. Further anaesthesia will be given directly into the toes being operated. This top-up is used to prolong the effects of the anaesthesia for 10–12 hours. You will therefore not be in any pain when you return home. When you are discharged from the clinic, you will be given a prescription for pain relief.
PERCUTANEOUS SURGERY :
Dr Lévy will perform the particular procedures needed by each patient (cheilectomy or arthrodesis) using micro-incisions for inserting instruments just 2mm in diameter. He does not touch the muscles, tendons or joint capsule. This means there is virtually no pain after the operation and patients can walk again immediately.
The scars will be barely visible to the naked eye. With a percutaneous technique, there is no need to detach the muscles, tendons or other structures in contact with the bone in order to perform the osteotomy. There is much less pain after the operation than with traditional surgery, and recovery is much faster.
Throughout the operation, the surgeon will take x-rays to check what is happening and make sure the osteotomy is as accurate as possible.
PERCUTANEOUS TRIMMING – CHEILECTOMY :
The dorsal exostosis (the bony bump protruding beneath the skin) is removed by making a tiny 2mm hole to shave off the bone using a miniature reamer. Progress is monitored using successive radioscopic images taken during the procedure. The aim is to stop the toe rubbing against the shoe and allow the joint to straighten again, so the patient can walk without a limp. The surgery will not address the osteoarthritis but will postpone the need for radical permanent treatment in the form of arthrodesis (joint fusion).
PERCUTANEOUS ARTHRODESIS :
The surgeon removes the small amount of remaining cartilage from the joint using a miniature reamer. Then the two bone surfaces are brought together and fixed in the correct position using two screws. The whole procedure is performed through three tiny 2mm incisions. The patient can go home the same day and walk pain-free.
Once finished, the surgeon will apply a compression dressing that will act as a splint for 8–10 days, during which you should not remove or loosen the bandage or get it wet.
You will then spend a few minutes in the recovery room so your vital signs can be monitored, after which you can return to your room and wait to be discharged.
Dr Lévy will prescribe any medication needed to alleviate any pain after the surgery. You will be discharged with your medical file explaining that you must bring back the dressings to your next check-up, along with any other instructions and the date and time of your next appointment when you will have another x-ray.
After being discharged, you will be able to walk with orthopaedic shoes that Dr Lévy will have prescribed for you during the preoperative consultation.
After the surgery
Dr Lévy will give you an appointment for a check-up in 8–10 days’ time. During this time, you must wear the orthopaedic shoes which are designed to relieve pressure on the forefoot.

POSTOPERATIVE CHECK-UPS :
8–10 DAY CHECK-UP :
Dr Lévy will remove the dressing, check the surface of the bone (after a cheilectomy) or the non-mobility of the joint (after arthrodesis). He will check the x-rays and make sure the wound is healing properly. After arthrodesis, he will give you a splint to keep the bones in place. This splint will make sure the bones heal in the correct position. You must wear it for 3 weeks. The dressings will be changed every three days until your next appointment. You must wear orthopaedic shoes for one month.
1-MONTH CHECK-UP :
The dressing and splint will be removed. You will return the orthopaedic shoes and can start wearing loose-fitting footwear (e.g. trainers, plimsolls). The swelling usually takes about 3 months to go down. Dr Lévy will give you compression bands which you must wear every day for three months after the operation. He will also give you some exercises (only after a cheilectomy) to help recover the full range of motion in your toes.
3-MONTH CHECK-UP :
This appointment is to check how your toes are healing. However, each case is different and you may be given advice on how to improve your condition and speed up your recovery.
You may also be given further appointments, if the surgeon thinks it is necessary.
REHABILITATION :
There is no physiotherapy after an arthrodesis because the aim of the surgery is to fuse the joint. You should therefore avoid trying to bend the joint.
With a cheilectomy (trimming), the aim of the surgery is to improve mobility in the joint. In most cases there is no need for rehabilitation therapy. At your first check-up appointment, Dr Lévy will give you some exercises to do at home. These exercises are designed to restore the range of motion in the joints, massage the scars to prevent any deep-seated adhesions, and get you walking again normally.
In some cases, he may want to prescribe you some sessions with a physiotherapist.
Potential complications
A wide range of complications can occur with surgery. Fortunately, they are very rare and the various appointments before and after the surgery are designed to avoid them or detect them early if they do appear.
As well as the risks common to all types of surgery and the risks of the anaesthesia, there are some specific risks associated with this procedure.
The following complications may occur with percutaneous surgery of the foot :
SURGICAL WOUND INFECTION :
Despite all the precautions taken by the operating team, bacteria may still enter the wound either during the surgery or afterwards, before it is fully healed. This causes compromised healing (redness around the wound), severe pain, a purulent discharge and a persistent fever.
You must tell the surgeon if you see any of these signs and seek emergency treatment.
NEURAPRAXIA :
During the operation, the surgeon will be working closely to the sensory nerves in the toes. If the instruments get too hot when close to these nerves, they may suffer a refractory period when feeling in one or more toes may lessen or disappear. This loss of feeling does not cause any problems when wearing shoes, and usually recovers within a year after the surgery.
DELAYED HEALING :
Sometimes, the bones take longer than three months to fuse. This is often the case with smokers who were unable to quit before, during and/or after the surgery due to the decreased blood flow to the toes. In these cases, Dr Lévy will give you advice on how to reduce pressure on the bones and help them heal faster.
COMPLEX REGIONAL PAIN SYNDROME :
Complex Regional Pain Syndrome, also known as algodystrophy, is a condition involving pain and other symptoms usually in a limb following trauma or surgery, even if only minor. The syndrome may have a neurological cause such as damage to the peripheral nervous system, affecting either the small fibres which protect from pain or heat stimuli, and/or the large fibres which detect tactile stimuli. It causes pain and severe stiffness in the rest of the foot that can last for up to 18 months. Patients always recover fully. Dr Lévy will diagnose the condition using scintigraphy (a scan) and will support you throughout, in order to treat the painful and unpleasant symptoms.
LOAD TRANSFER AND METATARSALGIA :
With some foot shapes (Greek foot, where the second toe is longer than the big toe), the change in loading pattern resulting from the surgery places excessive load on the second toe, causing plantar pain under the second metatarsal (metatarsalgia). This can be treated with orthopaedic insoles and further surgery to correct the excessive load. Dr Lévy should usually be able to detect this foot shape before the surgery and anticipate the load transfer to the second toe. However, this is sometimes not enough and the metatarsalgia can still occur.
PHLEBITIS/PULMONARY EMBOLISM :
Despite being able to walk again immediately, a clot may form in one of the veins of your leg (phlebitis) and require an effective dose of anticoagulant treatment for 3–6 months. This complication is rare with percutaneous surgery because the patient can walk again the same day.
This list does not cover all the possible risks.
Ask Dr Lévy if you want more information, especially if you have any questions about your particular situation and the advantages, disadvantages and risk/benefit ratio of each procedure.