Shoulder dislocation is both a very common and highly recurrent condition. It mostly affects athletes and is more frequent in young individuals or people with joint hyperlaxity. Early diagnosis and appropriate treatment are essential to limit complications and prevent recurrence.
Dislocation results in severe pain and the displacement of the shoulder either forward or backward. This joint can be unstable, as it is supported by muscles, tendons, and the glenoid labrum—a tissue that helps stabilize the contact between two bones. To prevent shoulder osteoarthritis, dislocation requires special attention, especially in the case of recurrence. Fortunately, shoulder dislocation can be treated very effectively today. Two surgical techniques may be considered depending on the case. If you suffer from shoulder dislocation or instability, this article will help you understand its causes, symptoms, treatments, and recovery.
What is a shoulder dislocation?
The shoulder is one of the most mobile joints in the human body, but also one of the most unstable. A dislocation occurs when the head of the humerus (upper arm bone) completely exits the glenoid cavity of the scapula. There are several types of dislocations:
- Anterior dislocation (most common, 95% of cases): the humerus shifts forward.
- Posterior dislocation (rarer, 5% of cases): the humerus moves backward.
- Inferior dislocation (extremely rare): the humerus moves downward from the joint.
What are the main causes?
Shoulder dislocation can be caused by:
- A violent trauma: such as falling on an outstretched arm, a sports accident, or a direct blow.
- Joint hyperlaxity: some individuals have more flexible ligaments, which increases the risk of repeated dislocations.
- A history of dislocation: a first dislocation increases the risk of recurrence, particularly in young athletes.
Why is shoulder dislocation prone to recurrence?
As mentioned, the shoulder joint is one of the most mobile. It is heavily used and therefore very unstable. Each episode of dislocation or subluxation (where the joint comes out and then returns to place) degrades the contact between the humeral head and the glenoid of the scapula. This leads to a loss of contact, directly impacting the joint and resulting in recurrence.
How to recognize a shoulder dislocation? Key symptoms
A shoulder dislocation presents with sudden and intense pain, often accompanied by an inability to move the arm. The joint may appear visibly deformed, giving the impression that the shoulder is “out of place.” In some cases, tingling or numbness may be felt in the arm if nerves are affected. In short, it is a rather painful condition that should not be taken lightly!
However, dislocation must be distinguished from subluxation, which characterizes shoulder instability. This instability can cause discomfort and pain, mostly of traumatic origin such as a misstep or fall. In these cases, a medical examination will determine whether the arm is still mobile and if strength is preserved. Untreated shoulder instability can worsen over time. Pain increases, range of motion decreases, and eventually leads to early shoulder osteoarthritis (omarthrosis).
Best practices in case of dislocation
When facing a shoulder dislocation, it is essential to act quickly and appropriately. One must never try to reposition the shoulder on their own, as it could worsen the injury. It is recommended to immobilize the arm against the body using a sling or fabric. Applying ice helps reduce inflammation. It is crucial to consult a doctor or go to the emergency room promptly for proper care.
Surgical intervention following a shoulder dislocation or instability
Shoulder dislocation is defined by very specific clinical signs and can be diagnosed quite easily. An X-ray and physical examination confirm the diagnosis.
Cases of subluxation and instability, however, require a more detailed and meticulous case study. X-rays of both shoulders will be prescribed, along with a CT arthrogram of the affected shoulder. In the case of more than two dislocation or subluxation episodes, surgery is recommended to prevent the development of osteoarthritis.
Two surgical treatments are possible depending on the case: arthroscopic treatment (Bankart technique) and open surgery (Latarjet technique).
Arthroscopic treatment
This minimally invasive technique involves inserting a camera and small surgical instruments through tiny incisions to repair damaged ligaments and stabilize the joint. This procedure results in two very small scars of about 5 mm, which become invisible after a few months. Arthroscopy allows for faster recovery compared to open surgery, with less postoperative pain and reduced risk of complications.
Open surgery
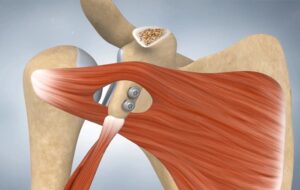
In more complex cases, when the damage is too severe or arthroscopy is insufficient to stabilize the joint, open surgery may be necessary. This procedure involves making a larger incision to access the joint directly and carry out more extensive repairs of the damaged structures. It may include placing a bone block, such as in the Latarjet technique, or repairing ligaments and the glenoid labrum. Although more invasive, this technique provides greater stability and is often preferred in severe recurring dislocations. The surgery involves a bone graft fixed with two small screws and usually leaves a 4 cm scar in the deltopectoral groove (area between the shoulder and the collarbone). Recovery is longer than with arthroscopy, with a more extended immobilization period, followed by progressive rehabilitation to restore mobility and muscle strength.
First pre-operative consultation
The first consultation with the surgeon aims to clearly establish the diagnosis and retrace the patient’s trauma history through a clinical interview. Dislocation? Subluxation? Instability? Each case is analyzed with precision, and depending on the lesions observed through radiological and arthroscopic exams, the surgeon will explain the procedure to follow. From the surgical act to potential complications, and through to recovery and rehabilitation, the first consultation details every step of the surgical intervention for shoulder dislocation.
Consultation with the anesthesiologist
After the pre-operative consultation with the surgeon, the patient meets with the anesthesiologist. The doctor examines the patient carefully and then explains how the anesthesia will proceed. Shoulder dislocation surgery is performed under general anesthesia combined with a regional block.
Note: It is essential to stop smoking one month before and one month after the surgery. Nicotine negatively affects blood circulation, which significantly impairs healing in the treated area.
Post-surgery follow-up
After surgery, the surgeon closely monitors the treated area. Following the operation, the patient must keep the arm in a sling at all times. During showers, the patient may remove the sling but must not move the arm away from the body. Depending on the case, passive rehabilitation sessions may be prescribed after about two weeks. For arthroscopic surgery, rehabilitation begins after one month.
Post-operative follow-up appointments
1st appointment: Day 30
At this first appointment, most patients no longer experience intense pain. However, the shoulder remains extremely fragile, and sleeping on it is prohibited. The surgeon checks the condition of the scars, and an X-ray is performed. Based on the imaging results, the doctor may prescribe active-assisted rehab sessions or increase the intensity of passive rehabilitation. Massaging the scars is recommended to reduce subcutaneous adhesions.
2nd appointment: Month 3
During the second appointment, the surgeon focuses on checking joint mobility. At this stage, patients typically regain between 90 and 120° of range of motion and are finally allowed to sleep on the operated shoulder. Joint strengthening rehab is prescribed, and daily stretching exercises at home are recommended by the doctor. For patients who underwent the bone block technique, an X-ray and a CT scan will be prescribed to verify the position of the graft.
Important information:
- Driving is not allowed for 30 to 45 days, depending on the type of surgery performed.
- If the patient has a manual job, they will be off work for at least 2 months (up to 4 months for physically demanding jobs).
If you have any concerns regarding your shoulder dislocation or instability, feel free to contact our team to schedule an appointment with Dr. Levy.